About infertility?
Infertility is the inability to conceive a child. Patients struggling with infertility are unable to get pregnant, even after having carefully timed, unprotected sex multiple times. There are safe and effective methods that can significantly improve one’s chances of getting pregnant. However, there are, sadly, still many women who still struggle to conceive.
What is recurrent pregnancy loss (RPL)?
The American Society of Reproductive Medicine defines recurrent pregnancy loss (RPL) as the loss of two or more pregnancies. RPL at a young age can be a way of determining whether a patient is experiencing infertility.

How common is infertility in women?
According to the Center for Disease Control and Prevention, 12% of women between, the ages 15 and 44 struggle with infertility in the US. This includes both getting pregnant and being able to carry a pregnancy.
Why is fertility so common?
The female reproductive system is a highly developed network. For a woman to be fertile, the ovaries must release healthy eggs. The egg must then pass through the fallopian tubes. Here, it will join with a sperm cell and develop into a healthy zygote. Even after the zygote forms, a woman’s reproductive system must provide and maintain a healthy environment in which the fetus can grow and develop. The complexity of such an evolved organ system leaves many areas for complications to arise. So, it may not be surprising to hear that over one in ten women struggles in conceiving before age 44.
Get a Second Opinion
Our endometriosis specialists are dedicated to providing patients with expert care. Whether you have been diagnosed or are looking to find a doctor, they are ready to help.Our office is located on 872 Fifth Avenue New York, NY 10065.
You may call us at (212) 988-1444 or have your case reviewed by clicking here.
Causes of infertility
A woman’s reproductive system and ovulation cycle is a very complex and carefully tuned network. Because of this complexity, infertility in women can result from a number of reasons. These include:
- ovulation disorders
- reproductive organ abnormalities
- reproductive organ damage or blockage
- early menopause
The following disorders can also cause or worsen infertility:
- endometriosis
- adenomyosis
- fibroids
- adhesions
- pelvic inflammatory disease
Risk factors for infertility
- Age: The older a woman gets, the more her egg quality declines. This drop in the number of healthy eggs is most noticed in a woman’s mid-30s. Though it is normal for infertility to arise at this age, if a patient is having trouble conceiving a child before their mid-30s, they should certainly seek to meet with a reproductive specialist, as they may be affected by any of the conditions listed above.
- Smoking/tobacco: Like with any health issue, smoking never helps. Cigarettes can have detrimental effects, and can physically damage your cervix, fallopian tubes, and ovaries. Research has shown that tobacco also decreases egg quality and quantity, and increases the risk of ectopic pregnancy. Though there is currently a lack of evidence to support that smoking can cause endometriosis, it clearly has a negative effect on fertility.
- Alcohol: Research has shown that women who consume an excessive amount of alcohol take longer to get pregnant, and have lower fertility rates and a higher chance of developing pregnancy complications. Alcohol aggravates endometriosis for a number of reasons, including liver dysfunctionality and increased levels of estrogen.
- Abnormal weight: both being underweight and overweight can cause a decrease in ovulation frequency and the likelihood of bearing a child.
Infertility and endometriosis
Nearly 50% of patients with endometriosis may experience infertility. It is important that you follow up with an infertility specialist or with your OB/GYN even after you have been treated for endometriosis.
How can endometriosis cause infertility?
Endometriosis may cause infertility in several possible ways. These include:
- alterations in prostaglandin secretion (a hormone-like enzyme, which can cause inflammation)
- the inability of the ovaries to function normally, resulting in a decrease in ovarian reserve and lack of egg production
- the body’s own impaired immune response, which can result in the rejection of the early implanted embryo and miscarriages
- anatomical distortions due to inflammation, adhesions, and/or scar tissue that prevent the proper passage of sperm to meet the egg
- improper or no implantation of the fertilized egg due to diffuse inflammation of the peritoneum
- cytokines in the serum of infertile women
How can endometriosis affect egg quality?
Research has shown that women who did not have endometriosis but used donor eggs from women with endometriosis had a much lower rate of achieving a healthy pregnancy. This suggests that women with endometriosis have a lower egg quality. This has been attributed to the presence of cytokines in the peritoneal fluid of patients with endometriosis, which is in fact caused by inflammation. The fluid will encase the healthy eggs and can affect them in such a way that they lose their function.
Endometriosis, immunity, and infertility
Endometriosis has an immune component that can lead to miscarriages due to excessive inflammation. This can cause the body’s immune system to reject the early implantation of the embryo. Therefore, it can be beneficial for a patient to seek an expert in reproductive immunology following any surgery to treat infertility, as they can help correct or strengthen a woman’s immune system in order to increase their chances of having a healthy pregnancy.
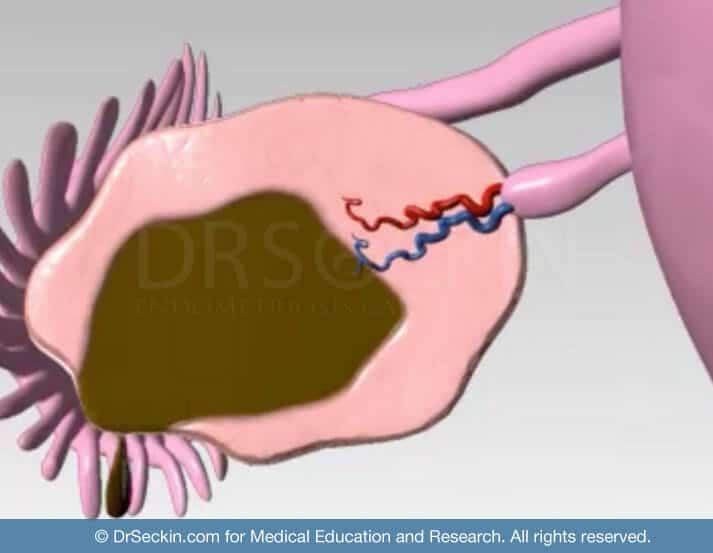
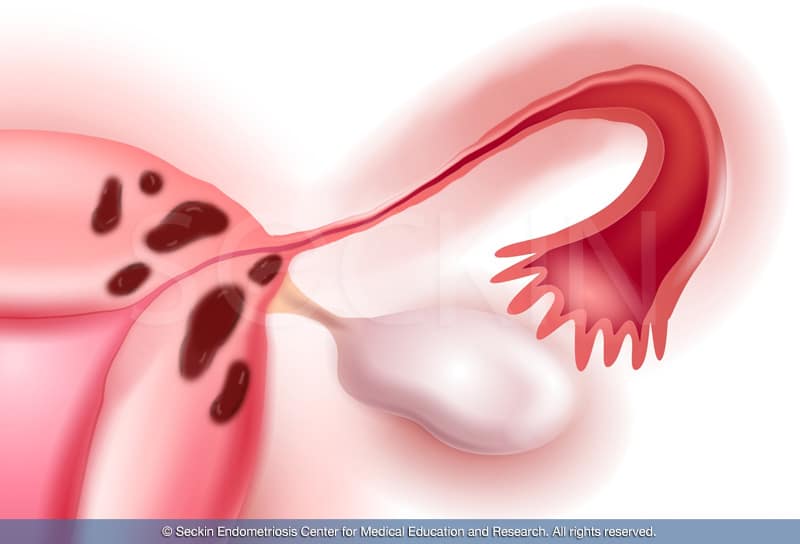
How does endometriosis lead to anatomical distortions that cause infertility?
The anatomical distortions that can arise from endometriosis can often lead to many pregnancy complications.
For example, scar tissue and adhesions that form on the fallopian tubes can lead to an ectopic pregnancy. An ectopic pregnancy is when the fertilized egg implants outside the uterus. In these cases, it is very important to terminate the pregnancy before the rupture of the tube.
Another example is the misshaping of the uterus due to associated adenomyosis scar tissue buildup and inflammation within the uterus. When this occurs, patients often have trouble maintaining a pregnancy.
It is important to consult a gynecological surgeon who can remove any of the scar tissue that causes these distortions in order to reduce inflammation and increase your chances of getting pregnant.
What is “silent endometriosis?”
Silent endometriosis refers to cases where patients with endometriosis are unsuccessful after multiple IVF courses but show no signs of endometriosis. Nevertheless, they continuously have multiple failed attempts with IVF treatments and are left undiagnosed for the cause of their infertility. This is why it is important to note that some women with endometriosis have no symptoms at all. In cases of infertility where there are no signs of endometriosis, patients should receive a laparoscopic evaluation of the pelvic peritoneum. This can eliminate inflammation as a possible cause of their infertility and ensure that they are not suffering from “silent endometriosis.”
How can patients overcome infertility due to endometriosis?

Endometriosis can reduce egg quality. We, therefore, advise that young patients with early endometriosis or a strong history of endometriosis freeze their eggs.
They may also need to have IVF treatment and preimplantation genetic testing in order to help achieve a healthy pregnancy. This also allows doctors to check the genetic makeup of the embryo and ensure it is genetically healthy. Only through transferring healthy embryos will patients gain a better chance of overcoming pregnancy loss.
Studies have also shown that women with endometriosis have a higher pregnancy success rate if they use frozen embryos rather than fresh eggs.
Diagnosing infertility
Because infertility is simply the inability to conceive children, as opposed to a visualizable disease, there is no way to concretely diagnose infertility without several failed attempts at pregnancy. Nevertheless, there are many diagnostic tools and methods that can be useful in diagnosing the underlying cause of infertility.
- Blood tests: A simple blood test can test whether or not a patient is ovulating properly by checking hormone levels.
- Hormone tests: There are many hormone tests that can help assess a patient’s chances of getting pregnant. These include ovulatory hormones, menstrual cycle hormones, and pituitary hormones that control reproductive processes. Any abnormal hormonal value can be a possible sign of infertility.
- Sonohysterography: This imaging technique uses an intravaginal ultrasound to produce images that evaluate the uterus and fallopian tubes. It can be used to find blockages, abnormal uterine bleeding, or any other causes of infertility.
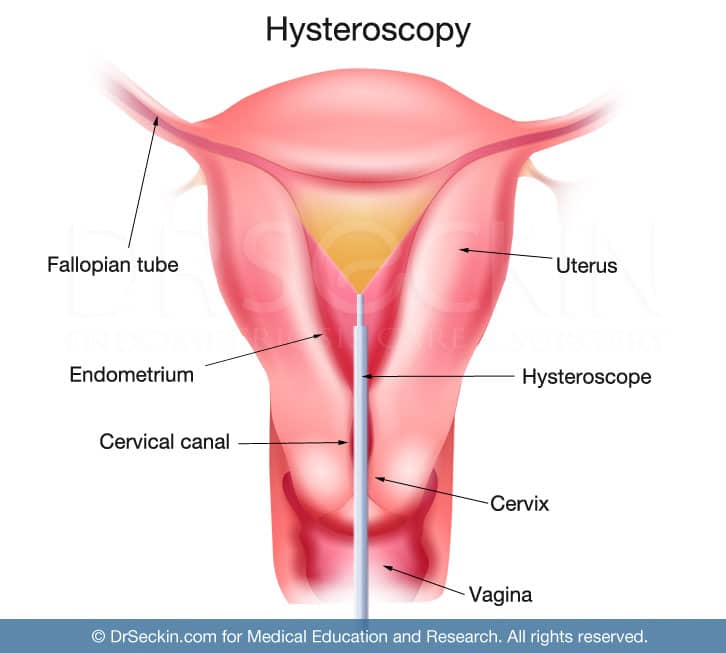
- Hysteroscopy: During this inpatient exam, the doctor inserts a thinly lighted device through the vagina in order to examine the cervix, inner uterus, and fallopian tubes. This can help determine if there are any causal diseases of infertility, such as endometriosis and adenomyosis.
- Laparoscopy: This is a minimally invasive surgical technique where the surgeon makes several small incisions into the abdomen. He or she then inserts a small camera to visualize the fallopian tubes, uterus, ovaries, and surrounding organs. In addition to its ability to visualize diseases such as endometriosis, adhesions, and blockages, laparoscopy is advantageous in that a surgeon will be able to remove any scar tissue they find. This allows laparoscopy to not only be a diagnostic tool for infertility but also as a form of treatment.
Treatment of infertility
The first step in the treatment of infertility is to determine its cause. Once the cause of infertility is established the best treatment course can be followed. This could be non-surgical or surgical.
Non-surgical
Fertility medications can help women with ovulation disorders. Stimulating ovulation through the use of key hormones, increases a woman’s chance of producing a greater quantity and quality of eggs. Women should discuss the risks and benefits of this approach with their doctor before starting treatment.
Surgical
Laparoscopic surgery can help diagnose certain causes of infertility and treat them. Using this approach, a surgeon can remove all ectopic endometrial tissue and adhesions. This can reduce inflammation and distortions of the uterus and other reproductive organs. This ultimately increases a patient’s chances of becoming pregnant.
Assisted reproductive technology (ART)
In some cases, a woman may need to use assisted reproductive technologies to become pregnant. These include Intrauterine insemination (IUI), in vitro fertilization (IVF), and third-party-assisted ART.
IUI: In this process, healthy sperm is placed directly into the uterus in order to ensure fertilization. This process will be properly timed with your menstrual cycle, whether it is normal or assisted by fertility medication.
IVF: This is by far the most common form of ART. In this technique, multiple mature eggs are stimulated and retrieved from a woman and fertilized in a petri dish with the sperm of the father. After a few days, the newly formed embryo is implanted back into the uterus.
Third-party assisted ART: There are a number of third-party assisted ARTs that are often used either alone or in congruence with any of the above ART techniques. These can include sperm donation, egg donation, surrogate, or gestational carrier. A surrogate is used when the woman in a couple is incapable of producing healthy eggs. In such cases, the sperm of the male partner must be used with a third-party female. A gestational carrier is used when the female simply cannot carry a pregnancy. Here, IVF is conducted using the mother’s egg and the father’s sperm. The resulting embryo is implanted into the uterus of the third party for pregnancy and delivery purposes.
Our approach
The best approach that we can provide in treating infertility is through laparoscopic deep excision surgery. By using this minimally invasive surgical technique, we are able to completely remove all visible endometriosis scar tissue in the uterus, ovaries, and surrounding reproductive organs. After the complete excision of endometriosis in the pelvis, all inflammation sources are eliminated. We will also surgically correct any observed uterine defects and free up the fallopian tubes in order to increase your chances of pregnancy. Together with some of the best reproductive endocrinologists and immunologists to offer you the best possible care. We have had a great number of patients go on to have healthy pregnancies. We pride ourselves on giving patients the highest chance of achieving a healthy pregnancy as we possibly can.
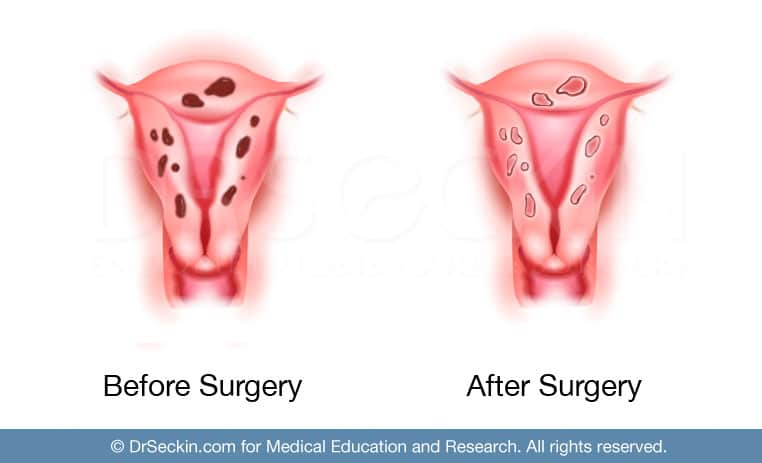
Nevertheless, endometriosis has been found to have an immune component that can lead to miscarriages even after surgical debulking. While our surgery greatly improves outcome, any patient who has gone on to become pregnant and miscarry, or those who have failed to conceive at all, should arrange for a reproductive immunology profile. This can be done by scheduling a reproductive immunologist follow-up meeting, which we are more than happy to help coordinate. If needed, we also recommend and can provide a referral to a clinic that provides ART.
It is important even after your surgery to keep in touch with us and consult with any necessary referrals, such as a reproductive immunologist or assisted reproductive technology (ART) clinics.
We want our patients to feel that they have options. While no one can guarantee a definitive cure for infertility, we do our absolute best in treating what is often the underlying cause of the disorder, ultimately making great improvements in a patient’s chances of bearing children. Patients are often unaware of just how impactful excision surgery can be in their particular case. We work extremely hard to provide the best possible care, while at the same time ensuring patients are not alone in this battle. Our door is always open for discussion to help patients with their family-building needs.
Patient story
When faced with the heartbreaking challenges of infertility, we believe male partners are as involved as their female partners. Here’s the story of an overjoyed husband from Great Neck who struggled to have a child with his wife for over five years, only to be blessed with a baby girl one year following his wife’s surgery. You can read more stories of patients overcoming infertility in our testimonial section.
Get a Second Opinion
Our endometriosis specialists are dedicated to providing patients with expert care. Whether you have been diagnosed or are looking to find a doctor, they are ready to help.Our office is located on 872 Fifth Avenue New York, NY 10065.
You may call us at (646) 960-3080 or have your case reviewed by clicking here.
Dr. Seckin is an endometriosis specialist and women’s reproductive health advocate. He has been in private practice for over 30 years at Lenox Hill Hospital with a team of highly skilled personnel.
Dr. Seckin specializes in advanced laparoscopic procedures and is recognized for his expertise in complex cases of deep infiltrating endometriosis of the pelvis. He is particularly dedicated to performing fertility-preserving surgeries on cases involving the ovaries.
He has developed patented surgical techniques, most notably the “Aqua Blue Excision” technique for a better visualization of endometriosis lesions. His surgical techniques are based on precision and microsurgery, emphasizing organ and fertility preservation, and adhesion and pain prevention.
Dr. Seckin is considered a pioneer and advocate in the field of endometriosis.
