Endometriosis is a painful condition that affects up to 10% of women of reproductive age and occurs when cells similar to those that line the uterus grows elsewhere in the body. One of the types of endometriosis is urinary tract endometriosis (UTE). It affects 0.3 to 12% of all endometriosis patients. Although the bladder is the most common site of UTE, bladder endometriosis, in general, is rare.
Bladder endometriosis can be superficial (only found on the surface of the bladder), or deeper and found on the inside of the bladder wall. Rarely, it can also affect the ureter, which is the muscular tube that connects the kidney to the bladder. Bladder endometriosis can also be either primary (occurring spontaneously) or secondary (occurring after pelvic surgery).
Causes of bladder endometriosis
The exact cause of bladder endometriosis is still not clear. Researchers developed several theories to explain the cause of the disease. One of these includes the migratory or metastatic theory. It proposes that retrograde menstruation causes products of the period to “go back” into the pelvis and implant in the bladder wall. This kickstarts the process of inflammation and adhesion with scarring that leads to endometriosis.
Symptoms of bladder endometriosis
As the location and size of bladder endometriosis can vary considerably from patient to patient, so do the symptoms.
A significant proportion of patients present with so-called urinary storage symptoms when first diagnosed. These can include bladder irritation, urgency, frequency, and painful symptoms when the bladder is full. Less commonly, patients report blood in the urine.
Importantly, the symptoms tend to occur cyclically with the menstrual cycle and are usually worse in the days leading to the period. As Dr. Seckin has stated, “if the symptoms are overlapping the periods, menstruation, before, during and after, certainly bladder endometriosis should be suspected.”
Get a Second Opinion
Our endometriosis specialists are dedicated to providing patients with expert care. Whether you have been diagnosed or are looking to find a doctor, they are ready to help.Our office is located on 872 Fifth Avenue New York, NY 10065.
You may call us at (212) 988-1444 or have your case reviewed by clicking here.
Diagnosis of bladder endometriosis
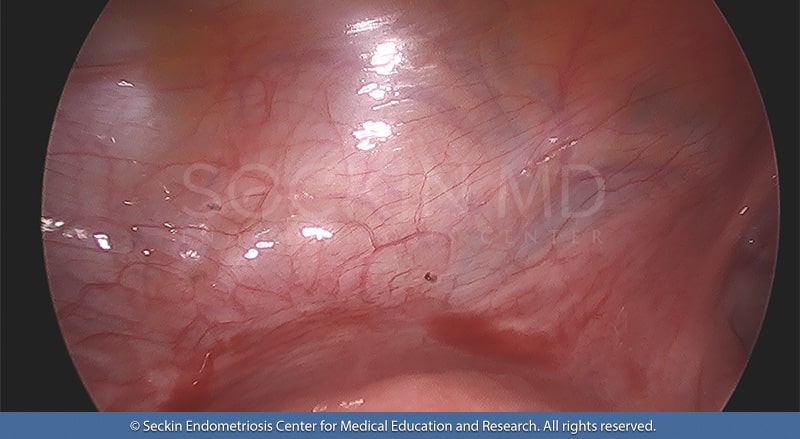
The diagnosis of bladder endometriosis often involves several steps. These may include a pelvic examination, cystoscopy (bladder examination), laparoscopy (abdomen/pelvic examination), computerized tomography (CT), and/or magnetic resonance imaging (MRI). As with pelvic endometriosis, surgical excision and pathology are the keys to a definitive diagnosis.
Treatment options
As with other types of endometriosis, the treatment of bladder endometriosis will depend on several factors. These include the patient’s age, fertility status and family planning preferences, the severity of the disease, the severity of urinary symptoms, and menstrual function.
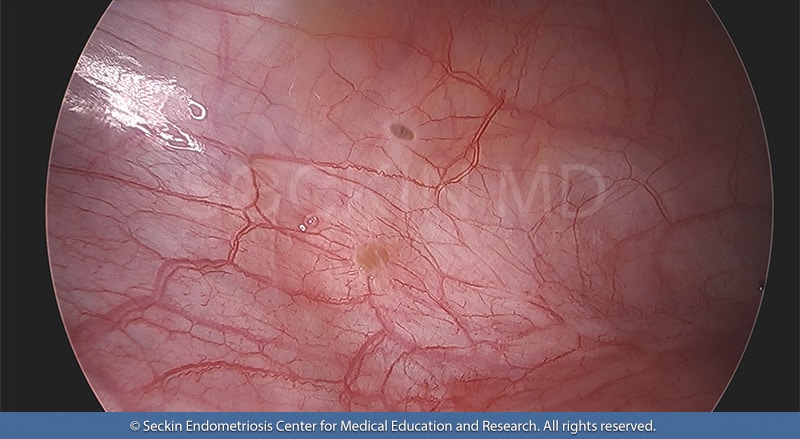
Treatment can be medical, surgical, or a combination of both. Medical treatments may involve pain medications and hormonal treatments that aim to reduce the progression of endometrial tissue. They include gonadotrophin-releasing hormone (GnRH) agonists and antagonists, progestins, and combined oral contraceptives. Surgical treatment options depend on the severity and area of the bladder affected and may include transurethral surgery (TUR), partial cystectomy, and/or a laparoscopic approach.
While medical treatments can help control the symptoms, they cannot cure the disease. Laparoscopic excision surgery conducted by an experienced surgeon is the gold standard treatment for bladder endometriosis like it is for other types of endometriosis.
Patient story
The road to a diagnosis is often long, as many patients with endometriosis may know. One such story is that of Winnie Chan, who spent years in and out of emergency rooms with no definite answers as to why she was in so much pain. Finally, after the worsening of her urinary symptoms and painful periods, she had an appointment with Dr. Seckin. She was diagnosed with advanced endometriosis, including advanced UTE. She underwent several surgeries in her long treatment journey. Read more about Winnie’s story.
Get a Second Opinion
Our endometriosis specialists are dedicated to providing patients with expert care. Whether you have been diagnosed or are looking to find a doctor, they are ready to help.Our office is located on 872 Fifth Avenue New York, NY 10065.
You may call us at (646) 960-3080 or have your case reviewed by clicking here.