Your Multidisciplinary Treatment Team for Endometriosis
Endometriosis is a chronic, progressive disease characterized by the growth of endometrial-like tissue outside the uterus. The normal endometrium, or the inner lining of the uterus, is shed during monthly periods. The extraneous endometrial outgrowths in endometriosis respond to female hormones just like the endometrium within the uterus. However, endometriosis growths (lesions) have no means of exiting the body. This results in pain and inflammation. These endometriosis lesions can deposit themselves in several areas such as the ovaries, fallopian tubes, bladder, and intestines. More rarely, they can even spread to the diaphragm, kidneys, and lungs. Therefore, a multidisciplinary treatment team for endometriosis is crucial for better outcomes and higher quality of life for the patient.
Why is a multidisciplinary treatment team for endometriosis necessary?
Endometriosis lesions often affect multiple organs. For example, deep infiltrating endometriosis (DIE) affects nearly 20% of all endometriosis patients. Lesions in DIE can penetrate 5 mm deep or more in the organs affected by the disease. Resecting larger DIE lesions requires extensive surgical expertise and a multidisciplinary approach coordinated by a skilled endometriosis surgeon. This increases the chance of a positive treatment outcome.
In 2019, the Society for Women’s Health Research involved a team of researchers, clinicians, and patients to deliberate on some of the barriers in current endometriosis treatment and management. The outcome of the review underscored that comprehensive, interdisciplinary approaches to disease management are necessary for the timely and accurate diagnosis and treatment of endometriosis.
What are the benefits of a multidisciplinary treatment team for endometriosis?
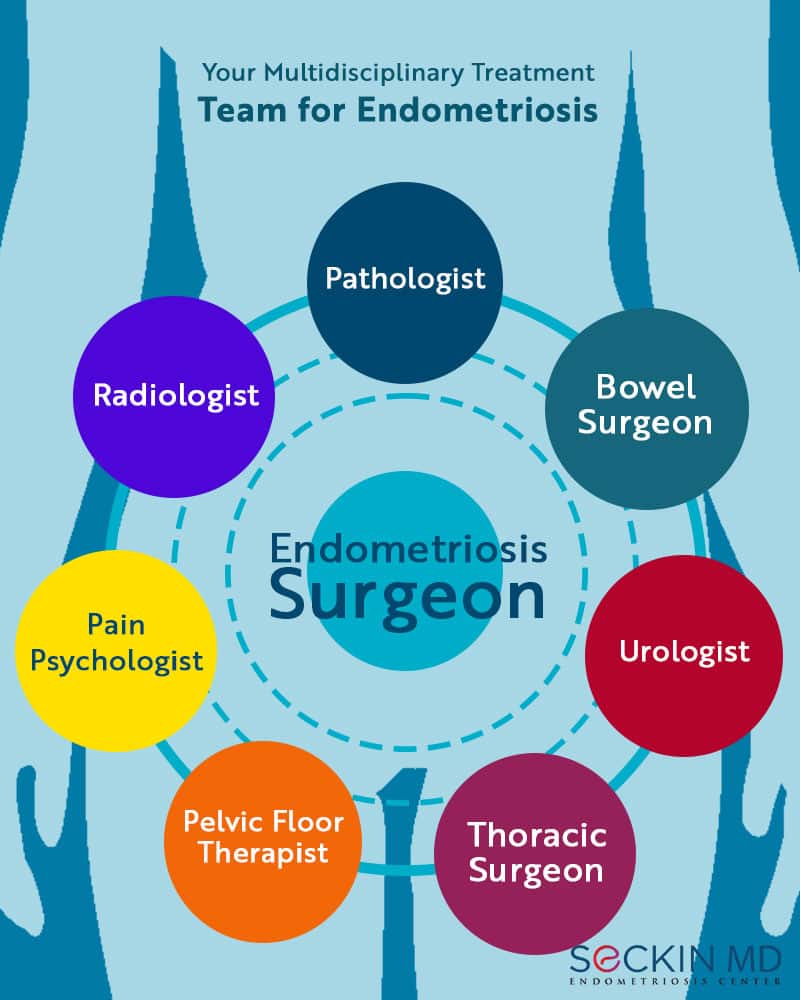
A multidisciplinary team (MDT) draws in specialists across various disciplines working together to enhance the patient’s treatment prospects and outcomes. An endometriosis MDT should comprise an endometriosis surgeon, a pathologist, a bowel surgeon, a urologist, a thoracic surgeon, a pelvic floor therapist, a pain psychologist, and a radiologist specializing in gynecology. The MDT team should collaborate at various levels to broaden the range of therapeutic intervention and management.
For instance, having a urologist in the team alongside the endometriosis surgeon can help in the better treatment of bladder and ureter lesions. It can also ensure the patient gets personalized advice on postoperative outcomes to minimize bladder or kidney complications. Similarly, having a pain psychologist on the team can help the patient with post-procedure coping strategies.
For clinicians, having a multidisciplinary approach provides a better framework for collaborative decision-making and implementation, particularly in complex cases. Cross-discipline learning, review, and research are only possible when several specialties work in unison.
Are there any studies demonstrating the effectiveness of a multidisciplinary approach?
Several case studies have indicated the importance and effectiveness of implementing a multidisciplinary approach for better outcomes. For example, the European Society of Human Reproduction and Embryology (ESHRE), in its endometriosis diagnosis and treatment guideline, emphasizes the need for an individualized, multidisciplinary approach to performing advanced laparoscopic surgery and laparotomy.
A 2016 study involving 87 women diagnosed with severe endometriosis evaluated the management outcomes of an MDT and the impact of surgical treatment on the patients’ quality of life. The results showed improvements in pain scores and improved quality of life, six and 12 months post-treatment. They also confirmed the benefits of streamlined, holistic patient management in a multidisciplinary setting enabling the women to make informed decisions between medical and surgical management.
An evaluation of three DIE cases in a 2021 case report highlighted the importance of thorough pre-operative planning by a multidisciplinary team comprised of subspeciality surgeons alongside the endometriosis specialist for optimal surgical outcomes. The case studies also concluded that patients with DIE would greatly benefit from centers that provide a multidisciplinary approach.
Our multidisciplinary treatment team for endometriosis
At Seckin Endometriosis Center (SEC) we have an MDT that collaborates on all aspects of treatment including pre-operative diagnosis, surgery, and post-operative recovery under the coordination of our endometriosis surgeon.
During diagnosis
Diagnosing endometriosis can be challenging. But a proper diagnosis can help determine the organs that the disease affects and which specialists the patient needs. We diagnose endometriosis using meticulous physical examination and spending time with the patient listening carefully to her symptoms. We sometimes use imaging techniques such as sonography, and magnetic resonance imaging (MRI). But the final diagnosis is only possible during the laparoscopic examination and post-surgical pathologic examination which is possible thanks to our excision approach.
Our MDT comprising a pathologist, radiologist, and other specialists can then discuss, review, and correlate the clinical findings. Endometriosis is a multi-organ disease. The MDT can assess individual organ dysfunction and extent of DIE on a per-lesion basis and plan for appropriate surgical intervention.
During surgery
Laparoscopic excision surgery is the gold standard for endometriosis treatment. Our aim is always to remove all endometriosis lesions while preserving reproductive function.
In cases of DIE, our MDT discusses the diagnostic findings and ramifications of performing these procedures with the patient. This enables her to make an informed decision before giving consent.
During post-operative recovery
Depending on the surgery, the post-operative experience can vary widely between patients. The pelvic floor therapist and pain psychologist provide the required support during recovery. They advise the patient on proper post-operative care for the sutures and common things that they can do at home during recovery.
At SEC, we also collaborate with support groups and complementary therapists such as physical therapists, mind-body interventionists, acupuncturists, recreational therapists, and dieticians to enable our patients to recover fast, stay motivated, and get back to their daily activities at the earliest.
What are some of the drawbacks or barriers to current multidisciplinary practices?
A formalized multidisciplinary approach is the best way to have increased positive therapeutic outcomes. But it is not always smooth sailing. An effective MDT would require higher levels of coordination, input, and cooperation among team members, not to mention collective accountability for the decisions made. Most MDT meetings do not involve the patients themselves. However, not involving patients in key decisions during the planning stage does bring with it the disadvantage of lack of proper input in the early stages of pre-operative planning. At SEC we always involve patients in key decisions.
Please feel free to share your experience with Seckin Endometriosis Center and comment on our post on Facebook or Instagram.
Get a Second Opinion
Our endometriosis specialists are dedicated to providing patients with expert care. Whether you have been diagnosed or are looking to find a doctor, they are ready to help.Our office is located on 872 Fifth Avenue New York, NY 10065.
You may call us at (646) 960-3080 or have your case reviewed by clicking here.