Dr. Seckin’s Lecture on Uterine Abnormalities at the First Global Congress on Hysteroscopy
Earlier this month on May 5th, Dr. Tamer Seckin, spoke at the Global Congress on Hysteroscopy in Barcelona, Spain. This was the first-ever meeting that discussed the findings of several board-certified hysteroscopic surgeons across the globe. Dr. Seckin’s lecture, entitled “Hysteroscopic Findings During Endometriosis Surgery,” was about uterine abnormalities and their effect on endometriosis.

About uterine abnormalities
Endometriosis is a disease that originates from the uterine cavity and spreads to other regions. For this reason, Dr. Seckin looks to examine the uterine cavity for malformations using hysteroscopy, in nearly each endometriosis surgery he performs.
Uterine abnormalities are structural abnormalities, which usually negatively affect uterine function, leading to both obstetric and gynecological issues. Therefore, uterine malformations are a highly important field of study amongst the hysteroscopy community. However, due to the wide range of different uterine abnormalities, these studies can vary in their findings.
Arcuate uterus is a subcategory of one of the most common forms of uterine malformations. Septate uteri are defined by a cavity-dividing the uterine septum. This septum derives from the narrow indentation of the fundus (top of the uterus) into the uterine cavity. Arcuate uteri are characterized by the same concave dip of the myometrium of the fundus into the uterine cavity but in a more subtle form.
But how does one make the distinction between these similar abnormalities? This brings up precisely where the conflict lies. In fact, most countries in Europe, simply do not make the distinction between septal and arcuate uteri. This may seem logical at first, as studies have shown arcuate uteri do not play a significant role in infertility, miscarriage, and other obstetric issues. Patients with a septate uteri, on the other hand, have a higher chance of miscarriage and overall infertility. However, some studies have shown that arcuate uterus, when explicitly defined, may play a role in certain gynecological conditions. For this reason, Dr. Seckin examines the effect of arcuate uterus and the role it plays in endometriosis patients.
Findings of scientific studies
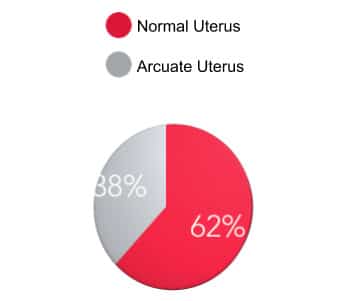
In a study of 260 endometriosis patients who received a hysteroscopy over two years, 100 had arcuate uterus, as defined by a previous study. This study differentiated arcuate uteri from septal uteri if the fundus did not exceed 1.5 cm of indentation. The other 160 patients had a normal uterus. While it only accounts for 38% of the patients, this is significant in comparison to the 3.8% of the general population with arcuate uterus according to another study. In other words, there seems to be a much higher prevalence of arcuate uterus in patients with endometriosis than in the general population. This brings up a key question: Could arcuate uterus play a causal role in the development of endometriosis?
Dr. Seckin’s surgery team uses a surgical technique to excise endometriosis that allows for a full pathology report for each patient. Using these reports, Dr. Seckin and his team identified the number of specimens that were pathologically confirmed to be endometriosis lesions. Of the 100 arcuate uteri endometriosis patients, 39 were positive for endometrioma development (39%). This was much larger in proportion to the 38 positive endometriomas out of the 160 normal uteri endometriosis patients (24%). This meant that having a uterine anomaly, specifically arcuate uterus, brought a 1.76 fold greater chance of ovarian endometrioma, which can even lead to multiple organ involvements and the presence of stage 3 or 4 endometriosis. Thus Dr. Seckin’s study led to two main findings.
First, patients with an arcuate uterine cavity have a statistically higher chance of being positive for endometriosis. And second, patients with an arcuate uterine cavity will also have a higher chance of pathologically testing positive for an endometrioma, than those with a normal uterine cavity. So, how can this information play a role in future endometriosis treatment?
Importance of distinguishing arcuate and septate uteri
Making the distinction between arcuate uterus and septate uterus is crucial as it shows that what one uterine abnormality may mean for an obstetric patient may be different in the case of endometriosis. Thus, the identification of whether or not a patient has arcuate uterus through hysteroscopy should be a key step in any endometriosis surgery case. It also raises the idea that a potential resection of midline prominence and restructuring of the uterine cavity to its normal anatomical structure, may be a significant step for the surgical treatment of endometriosis.
Get a Second Opinion
Our endometriosis specialists are dedicated to providing patients with expert care. Whether you have been diagnosed or are looking to find a doctor, they are ready to help.Our office is located on 872 Fifth Avenue New York, NY 10065.
You may call us at (646) 960-3080 or have your case reviewed by clicking here.